Common Procedures
Gum Disease | Extractions | Fillings | Root Canals
Preventing Gum Disease
Gum disease (also called periodontal disease) is an infection of the tissues that support your teeth. It is a major cause of tooth loss in adults. Because gum disease is usually painless, you may not know you have it. At each regular checkup the dentist will measure the depth of the shallow v-shaped crevice (called a sulcus) between your tooth and gums to identify whether you have gum disease.
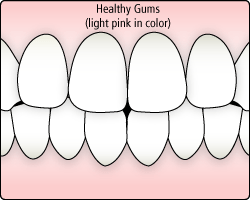
Gum disease is caused by plaque, a sticky film of bacteria that constantly forms on the teeth. These bacteria create toxins that can damage the gums.
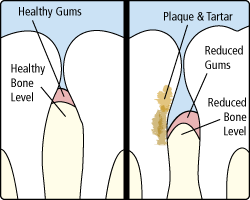
Periodontal diseases attack just below the gum line in the sulcus, where they cause the attachment of the tooth and supporting tissues to break down. As the tissues are damaged, the sulcus develops into a pocket; generally, the more severe the disease, the greater the depth of the pocket.
Periodontal diseases are classified according to the severity of the disease. The two major stages are gingivitis and periodontitis.
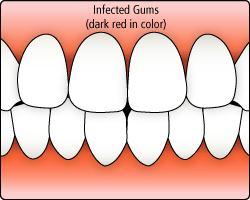
Gingivitis
In the early stage of gum disease, called gingivitis, the gums become red, swollen and bleed easily. At this stage, the disease is still reversible and can usually be eliminated by daily brushing and flossing.
Periodontitis
In the more advanced stages of gum disease, called periodontitis, the gums and bone that support the teeth become seriously damaged. Whereas healthy gums and bone anchor teeth firmly in place, infected gums can cause teeth to become loose, fall out, or have to be removed by a dentist.
Some factors increase the risk of developing periodontal disease:
- Tobacco smoking or chewing
- System-wide diseases such as diabetes
- Some types of medication such as steroids, some types of anti-epilepsy drugs, cancer therapy drugs, some calcium channel blockers, and oral contraceptives
- Bridges that no longer fit properly
- Crooked teeth
- Fillings that have become defective
- Pregnancy
If you notice any of the following signs of gum disease, see the doctor immediately:
- Gums that bleed easily
- Red, swollen, tender gums
- Gums that have pulled away from the teeth
- Persistent bad breath or bad taste
- Pus between your teeth and gums
- Permanent teeth that are loose or separating
- Any change in the way your teeth fit together when you bite
- Any change in the fit of partial dentures
It is possible to have periodontal disease and have no warning signs.
That is one reason why regular dental checkups and periodontal examinations are very important. Treatment methods depend on the type of disease and how far the condition has progressed.
Good oral hygiene at home is essential to keep periodontal disease from becoming more serious or recurring. You don't have to lose teeth to periodontal disease. Brush regularly, clean between your teeth, eat a balanced diet, and schedule regular dental visits for a lifetime of healthy smiles.
Extractions
There are times when it is necessary to remove a tooth. Sometimes a baby tooth has misshapen or long roots that prevent it from falling out as it should, and the tooth must be removed to make way for the permanent tooth to erupt. At other times, a tooth may have so much decay that it puts the surrounding teeth and jaw at risk of decay, so your doctor may recommend removal and replacement with a bridge or implant. Infection, orthodontic correction, or problems with a wisdom tooth can also require removal of a tooth.
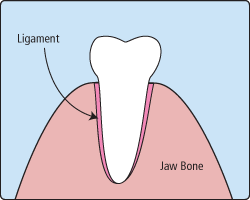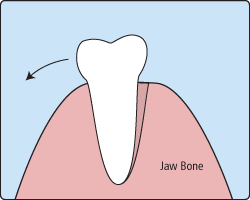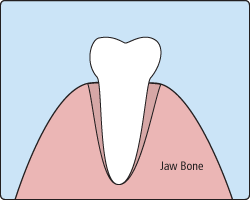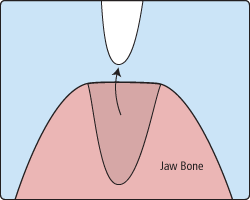
When it is determined that a tooth needs to be removed, your dentist may extract the tooth during a regular checkup or may request another visit for this procedure. The root of each tooth is encased within your jawbone in a "tooth socket," and your tooth is held in that socket by a ligament. In order to extract a tooth, your dentist must expand the socket and separate the tooth from the ligament holding it in place. While this procedure is typically very quick, it is important to share with your doctor any concerns or preferences for sedation.
Once a tooth has been removed, neighboring teeth may shift causing problems with chewing or with your jaw joint function. To avoid these complications, your dentist may recommend that you replace the extracted tooth.
Fillings
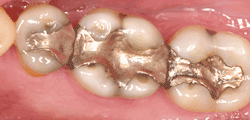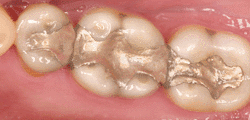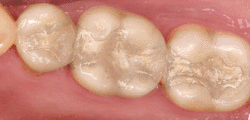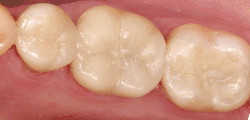
Traditional dental restoratives (fillings) include gold, porcelain, and composite/amalgam. The strength and durability of traditional dental materials continue to make them useful for situations where restored teeth must withstand extreme forces that result from chewing, such as in the back of the mouth.
Newer dental fillings include ceramic and plastic compounds that mimic the appearance of natural teeth. These compounds, often called composite resins, are usually used on the front teeth where a natural appearance is important. They can be used on the back teeth as well depending on the location and extent of the tooth decay. Composite resins are usually more costly than the older silver amalgam fillings.
What's Right for Me?
Several factors influence the performance, durability, longevity and expense of dental restorations:
- The components used in the filling material
- The amount of tooth structure remaining
- Where and how the filling is placed
- The chewing load that the tooth will have to bear
- The length and number of visits needed to prepare and adjust the restored tooth.
The ultimate decision about what to use is best determined in consultation with your doctor. Before your treatment begins, discuss the options with your doctor. To help you prepare for this discussion it is helpful to understand the two basic types of dental fillings: direct and indirect.
- Direct fillings are fillings placed immediately into a prepared cavity in a single visit. They include dental amalgam, glass ionomers, resin ionomers, and composite (resin) fillings. The dentist prepares the tooth, places the filling, and adjusts it during one appointment.
- Indirect fillings generally require two or more visits. They include inlays, onlays, veneers, crowns, and bridges fabricated with gold, base metal alloys, ceramics, or composites. During the first visit, the dentist prepares the tooth and makes an impression of the area to be restored. The dentist then places a temporary covering over the prepared tooth. The impression is sent to a dental laboratory which creates the dental restoration. At the next appointment, the dentist cements the restoration into the prepared cavity and adjusts it as needed.
Root Canal (Endodontic) Treatment
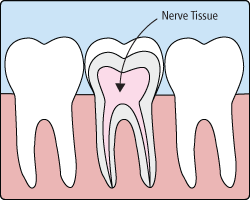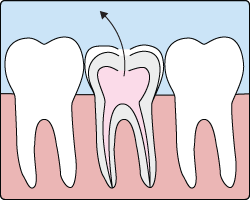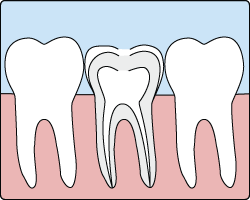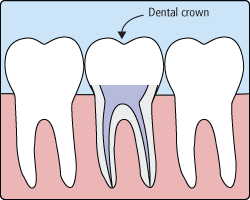
In the past, if you had a tooth with a diseased nerve, you'd probably lose that tooth. Today, with a special dental procedure called root canal treatment, you may save that tooth.
Inside each tooth is both the pulp and the nerve. The nerve is the vestige of the tissue that originally formed the tooth. Once the tooth has been in the mouth for a time, the functioning of the nerve is no longer necessary.
When a tooth is cracked or has a deep cavity, bacteria can enter the pulp. Germs can cause an infection inside the tooth. Left without treatment, pus builds up at the root tip in the jawbone, forming a "pus-pocket" called an abscess. An abscess can cause the pulp tissue to die. When the infected pulp is not removed, pain and swelling can result. Certain by-products of the infection can injure your jawbones and your overall health. Without treatment, your tooth may have to be removed.
Treatment often involves from one to three visits. During treatment, your general dentist or endodontist (a dentist who specializes in problems of the pulp) removes the diseased pulp. Next the pulp chamber and root canal(s) of the tooth are cleaned and sealed. Often posterior teeth that have endodontic treatment should have a cast crown placed in order to strengthen the remaining structure. Then, as long as you continue to care for your teeth and gums with regular brushing, flossing, and checkups so that the root(s) of the restored tooth are nourished by the surrounding tissues, your restored tooth can last a lifetime.
Most of the time a root canal is a relatively simple procedure with little or no discomfort, involving one to three visits. Best of all, it can save your tooth and your smile!
